Rehabilitation Techniques for Paralysis from Stroke, SCI or TBI
Paralysis treatment is one area within the healthcare industry that necessitates the use of specialized rehabilitation techniques. There is a particularly substantial evidence base to support the interventions therapists use to address paralysis. Many of these are aimed at improving upper extremity function, increasing mobility, and preventing further injury.
An individual may experience paralysis as a result of a cerebrovascular accident (also known as a CVA, or a stroke), a traumatic brain injury (TBI), or a spinal cord injury (SCI) (National Library of Medicine, 2016). Paralysis may also occur due to chronic conditions such as amyotrophic lateral sclerosis (ALS), or autoimmune disorders such as Guillain-Barre syndrome.
Therapists may use any combination of interventions based on a person’s diagnosis and presenting needs. In this article, we will review a few of the most widely respected techniques and the evidence that supports their use in practice.
Neuromuscular Stimulation and Functional Electrical Stimulation
Functional electrical stimulation (FES) involves sending electrical impulses to fully or partially paralyzed muscles to create a contraction. By placing electrodes on the skin, therapists can use these impulses to encourage participation in functional tasks such as brushing teeth, buttoning a shirt, writing a sentence, and putting on a jacket. This modality has been in use since the 1960s, which speaks to its efficacy in the rehabilitation process for paralysis.
Research demonstrates FES can improve an individual’s active range of motion after stroke and SCI (Howlett et al., 2015) as well as increase functional upper extremity use for activities of daily living such as dressing, eating, and bathing (Eraifej et al., 2017), and assist in walking (Popovic et al., 2001). In addition, the evidence shows this modality is most effective when provided within the first 2 months after an injury, as this window is when the brain has the most potential for change.
Neuromuscular stimulation, or NMES, has the same mechanism as FES does. However, the impulses associated with NMES last longer and are more powerful than those of FES. This is because FES is intended to generate a contraction to help someone complete a functional task (e.g. grasping a pen or moving a toothbrush) and then allow the muscle to relax. NMES, on the other hand, sends much more energy to the affected muscle over a longer period of time to produce a reaction in the brain in preparation for movement of any kind. So you can think of FES as giving purposeful electrical impulses, while NMES offers preparatory impulses.
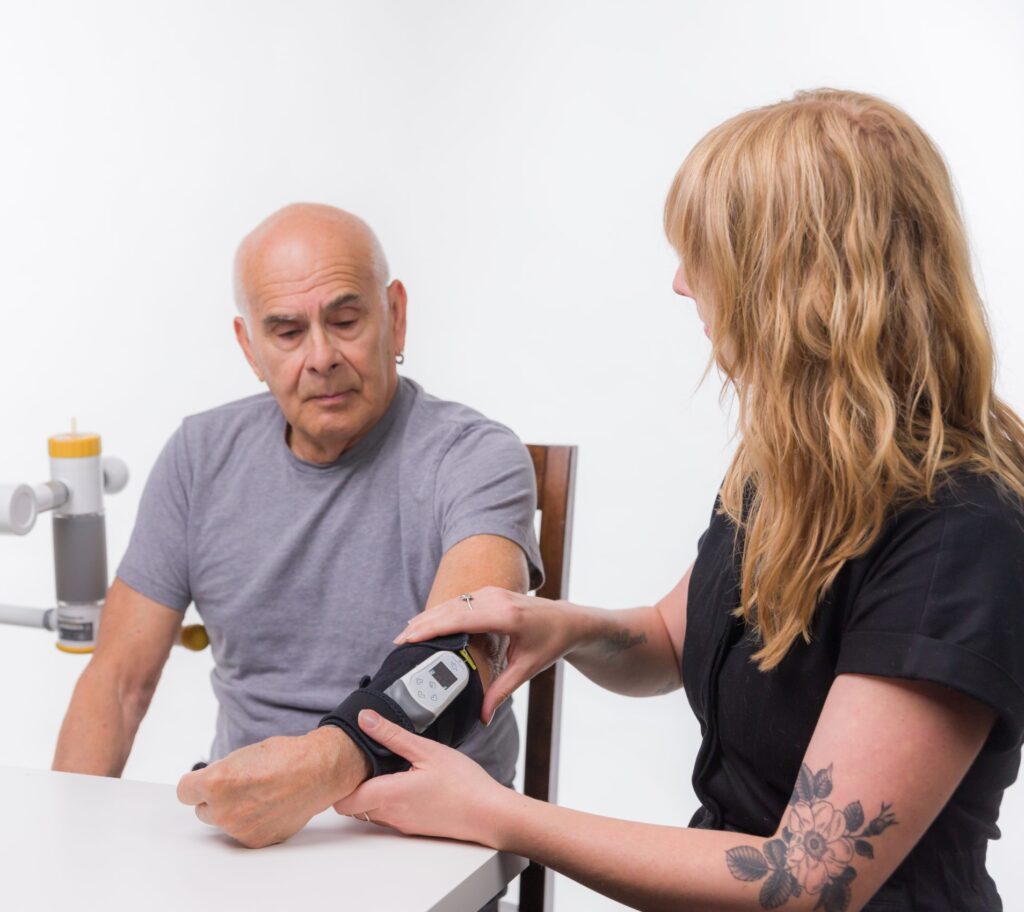
ReGrasp hand neurorehabilitation system is an innovative Rehabtronics device that utilizes this technology. ReGrasp uses FES to improve hand range of motion and function while improving blood flow, reducing muscle spasms, and offering a host of other benefits.
Interested in learning about how FES can help you regain hand function? Read more.
Virtual Reality Rehabilitation Programs
Virtual reality (VR) uses simulated engagement in 3D to offer individuals an immersive experience in a novel, unique environment. VR can be used for entertainment, but the healthcare industry has harnessed its power in creating individualized rehabilitation programs for a range of conditions. In particular, VR rehabilitation programs are an engaging way to help individuals improve upper or lower body coordination, balance, strength, and motion after paralysis. Virtual reality is often a part of comprehensive rehabilitation programs, as it can also assist with improving cognition and building other skills.
In fact, one study found that a six-week VR rehabilitation program lowered fatigue rates in veterans living with paralysis (Pourjafari et al., 2022). Other research shows that virtual reality programs have been effective in improving upper extremity limb function (specifically grip strength, pinch strength, and use of the palm) in individuals with SCI (Lim et al., 2020). A large-scale review also found that VR programming has shown beneficial for gait, balance, posture, and upper extremity motor function in individuals with Parkinson’s disease. This review also found that many individuals sustained these motor gains several months after their programs ended (Amirthalingam et al., 2021).
While more research is needed to determine the full extent of skills that may benefit from VR programs, evidence suggests they have been effective thus far in assisting with paralysis and related motor concerns.
Mirror Therapy
Mirror therapy is specifically used for stroke rehabilitation, as it uses a person’s uninjured arm to assist their injured arm in relearning normal movement. This treatment uses only a mirror placed at the body’s center in such a way that it reflects an image of the person’s uninjured arm. While moving this unaffected arm as one normally would, an individual is sending signals of “typical” movement to their brain. This stimulates brain cells called mirror neurons, which helps in the recovery process.
A large review on mirror therapy showed a significant positive effect on motor function in individuals who sustained a stroke. This review included studies that described three to seven sessions of mirror therapy per week, each lasting 15 to 60 minutes for a total of two to eight weeks. While there were a few variations between the studies, they were beneficial for optimal outcomes with mirror therapy. This review found that mirror therapy was also advantageous for reducing pain and improving participation in activities of daily living (Thieme et al., 2018).
Mirror therapy also has a track record of positive effects when used with a pediatric population. A few researchers looked at its use in children with cerebral palsy. One study found that children who regularly received mirror therapy experienced improved movement speed, hand strength, greater muscle activity, and better accuracy of hand matching (Park et al., 2016).
Summary
Each of these modalities has proven successful in treating individuals with paralysis. Additional interventions that may help someone regain motion include constraint-induced movement therapy, therapeutic massage, and adaptive equipment such as wearable orthotics. Each of these treatments can be provided by qualified rehabilitation professionals called physical therapists and occupational therapists. If you are interested in learning more, speak to your physician to get the therapy process started.
References:
- National Library of Medicine – MedlinePlus. (2016). Paralysis. Retrieved from https://medlineplus.gov/paralysis.html
- Howlett, O.A., Lannin, N.A., Ada, L., & McKinstry, C. (2015). Functional Electrical Stimulation Improves Activity After Stroke: A Systematic Review With Meta-Analysis. Archives of Physical Medicine and Rehabilitation, 96(5), 934-943. https://doi.org/10.1016/j.apmr.2015.01.013.
- Eraifej, J., Clark, W., France, B., Desando, S., & Moore, D. (2017). Effectiveness of Upper Limb Functional Electrical Stimulation After Stroke for the Improvement of Activities of Daily Living and Motor Function: A Systematic Review and Meta-Analysis. Syst Rev, 6(40). https://doi.org/10.1186/s13643-017-0435-5
- Popovic, M., Curt, A., Keller, T., & Dietz, V. (2001). Functional Electrical Stimulation for Grasping and Walking: Indications and limitations. Spinal Cord, 39, 403–412. https://doi.org/10.1038/sj.sc.3101191
- Pourjafari Jorjafaki, B., Hovanloo, F., & Mohammadi, F. (2022). Effect of Six Weeks Virtual Reality-Based Rehabilitation Exercise and Reflexology on Fatigue Rate of Paralyzed Veterans. Iran J War Public Health, 14(1), 19-24. http://ijwph.ir/article-1-1071-en.html
- Lim, D.Y., Hwang, D M., Cho, K.H., Moon, C.W., & Ahn, S.Y. (2020). A Fully Immersive Virtual Reality Method for Upper Limb Rehabilitation in Spinal Cord Injury. Annals of Rehabilitation Medicine, 44(4), 311–319. https://doi.org/10.5535/arm.19181
- Amirthalingam, J., Paidi, G., Alshowaikh, K., Jayarathna, A.I., Manisha R. Salibindla, D.B.A., Karpinska-Leydier, K., & Er, H.E. (2021). Virtual Reality Intervention to Help Improve Motor Function in Patients Undergoing Rehabilitation for Cerebral Palsy, Parkinson’s Disease, or Stroke: A Systematic Review of Randomized Controlled Trials. Cureus, 13(7), e16763. DOI 10.7759/cureus.16763
- Thieme, H., Morkisch, N., Mehrholz, J., Pohl, M., Behrens, J., Borgetto, B., & Dohle, C. (2018). Mirror Therapy for Improving Motor Function After Stroke. The Cochrane Database of Systematic Reviews, 7(7), CD008449. https://doi.org/10.1002/14651858.CD008449.pub3
- Park, E.J., Baek, S.H., & Park, S. (2016). Systematic Review of the Effects of Mirror Therapy in Children with Cerebral Palsy. Journal of Physical Therapy Science, 28(11), 3227–3231. https://doi.org/10.1589/jpts.28.3227